Developing a Draft Model to be Utilized as a Framework for a Logic Model to Evaluate the Social Values of Programs and Projects in the Field of Healthcare
- Social impact measurement
- Logic model
- Outcome
- Health behavior
- Social issues
As a variety of social issues have been noticed in recent years, various programs and projects are now conducted to resolve the issues. In many cases however, whether these programs and projects have been effective is actually not evaluated. Under this circumstance, Social Impact Measurement is attracting attention as a method to visualize the benefit of programs and projects. The Social Impact Management Initiative permeates Social Impact Measurement widely in society and promotes solutions for social issues.
In this study, we developed a draft model as part of the activities, which is to be utilized as a framework for a logic model in the healthcare field. Such a logic model illustrates the causes and effects between individual elements from input to outcome in the programs and projects, which is to be needed for Social Impact Measurement.
Based on health behavior theories and models, a draft model has been developed in this study, specifically focusing on one’s behavior change. The draft model is expected to be utilized to develop a logic model for healthcare-related programs and projects, applications, and healthcare devices.
1. Introduction
1.1 Background
Various programs and projects are underway to resolve the various social issues that have recently surfaced. Such efforts often fail to be evaluated for effectiveness in resolving actual social issues. In this context, social impact measurement has come to attract much attention as a method of visualizing the social value of programs or projects.
Taking note of logic models as social impact measurement tools, we created a draft model usable as a template for creating logic models for healthcare-related programs (or projects). Note, however, that we limited our scope to healthcare in a sense to be defined later, excluding such areas as frailty prevention, for instance. Besides, in the present study, we attached importance to making healthcare programs more effective for individual care recipients. Therefore, this paper mainly revolves around individuals’ behavior changes from the perspectives of health behavior theories and avoids directly discussing such matters as benefits for organizations. This study’s scope and prerequisites are to be presented later.
1.1.1 Social impact measurement
Social impact measurement is a process of making value judgments on a program or a project through the quantitative and qualitative understanding of the “social and environmental changes, benefits, lessons learned, and other effects” resulting from it over the short or long term1). “Measurement” does not mean either “auditing” or “assessment” but “derivation of values” and provides various advantages, such as organizational growth or improvement of the program or project2).
Social impact measurement is divided mainly into four stages (planning, implementation, analysis, and reporting/utilization stages). The Planning Stage consists of four steps (Step 1 “Preparation for practice,” Step 2 “Logic model creation,” Step 3 “Selection of the outcome to be evaluated,” and Step 4 “Determination of the indicator/measurement method”). In the Implementation Stage, an indicator decided on in the Planning Stage is used for data collection. In the Analysis Stage, the collected data provides the basis for analyzing expected results, challenges, impediments, and other factors. In the Reporting/Utilization Stage, the analysis results are used to improve the program or project1).
The Social Impact Management Initiative (hereafter SIMI) is a multisector initiative for promoting widespread use of social impact management all over Japan through cooperation among the various members in Japan, including operators, funders, intermediaries, government, intermediate support organizations, think tanks, evaluators, and researchers. When our draft model was under development, SIMI was pursuing its activities with a vision of getting social impact measurement widely rooted in society by 2020 to help resolve social issues3). We participated in an activity selected as one of the activities under the Working Group for Healthcare-Field Outcomes and Indicators through public solicitation in 2018. In this activity, we created a support tool for the social impact measurement planning stage. Regarding the activity, this paper contains a part corresponding to Step 2 “Logic model creation” mentioned above. A logic model provides a social impact measurement tool. Its creation is the phase of introducing social impact measurement.
1.1.2 Logic model
A logic model shows the cause-and-effect chain among individual elements of a program in the flow of events up to the program’s improving social conditions4). The term “program” in the sense used here refers to an entire effort to produce a social effect5), which consists of the “input,” “activity,” “output,” and “outcome” in a logic model. An “input” is a resource used to perform various activities in a program. This paper uses the term “various activities” to refer to any “activity” performed to provide a product, a service, or other offerings. A product, a service, or an offering provided through an “activity” is an “output.” A change or an effect resulting from an “output” is an “outcome.” The purpose of a program or an organization is to produce this change or effect6). Generally, an outcome falls into one of the following three levels set in the order of proximity to the output: “short-term outcome,” “intermediate outcome,” and “long-term outcome.”1)
The utilization of a logic model allows the logical organization and improvement of elements necessary to make a program more effective in the flow of steps from planning through implementation to the evaluation of its effects7).
1.2 Significance of creating a draft logic model for programs in the healthcare field
Typical logic models used in the healthcare field, including self-health control and disease prevention, include those for the gymnastics class program provided by General Incorporated Association RePlus8) and the anti-locomotive classes held in Kanagawa Prefecture9). Logic models are also used in the medical fields, including emergency medicine, pediatric medicine, and measures for cancers and cerebral strokes10,11). Logic model creation procedures1,6,7) have been presented by various organizations, and workshops have also been hosted for logic model creation12). However, generally, logic model creation assumes related knowledge and experience and requires considerable time and effort. Hence, these points may pose impediments to logic model-based social impact measurement efforts.
The draft logic model created in this study aimed at reducing the workload of logic model creation in the healthcare field. This paper presents the components of our model, along with the health behavior theories and model providing its basis, aiming to allow easier creation of logic models with their elements increased, decreased, or modified to suit the nature of the programs. Our draft model will simplify the processes involved in healthcare-related program logic model creation and require a smaller workload than required to create one from scratch. Besides, we expect that as a result, social impact measurement efforts will be promoted for various healthcare-related programs or services, apps, health devices, and the like.
1.3 Our study’s scope
This study’s draft logic model was created from the evaluation perspective for the scope presented below.
1.3.1 Prerequisites for the draft logic model
The types of programs within the scope of this study were programs aiming at health promotion or lifestyle-related disease prevention through the use of healthcare-related products or services. This study excluded medical services, pharmaceutical products, and medical equipment from its scope and did not cover treatments for individual diseases. The definition of “healthcare” is to be given in the next subsection.
Program beneficiaries (eligible support recipients) were specified as participants in the target programs (individuals). The long-term outcome of a target program was specified as extended healthy life expectancy. We consider the specification of this outcome as appropriate, considering that expectations have been running high for health promotion services and lifestyle-related disease prevention services in recent years and that efforts have been underway to extend healthy life expectancy13,14).
The assumed users of our model are those involved in target programs, such as program planners, implementers, and evaluators. The assumed evaluators are not limited to internal evaluation personnel but include third parties performing external evaluations.
1.3.2 Healthcare as defined for this study
The scope of healthcare in this study was defined as follows based on the prerequisites presented in the subsection immediately above (Fig. 1):
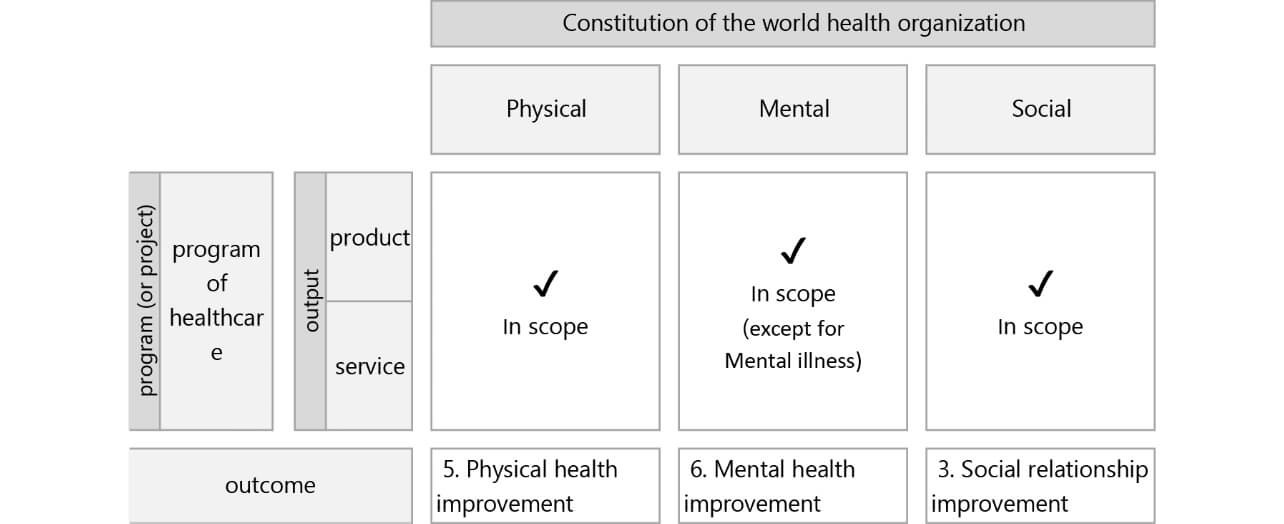
The WHO Constitution defines health as “a state of complete physical, mental, and social well-being and not merely the absence of disease or infirmity.”15) Based on this definition, healthcare in the sense defined for this study covered health in the physical, mental, and social domains, excepting mental illnesses and disorders included in the mental domain because these areas require care and treatment specialty and hence fall outside this study’s scope. We also decided to exclude other individual illnesses, which require specialist medical interventions, from our study’s scope.
It is commonly accepted that continued healthy behaviors are necessary to prevent the occurrence and worsening of many diseases, including lifestyle-related diseases, and to treat them16,17). Accordingly, the draft model we created had its focus on the perspectives of health behavior theories, including health-related behavior changes. Subsection 2.2 outlines several health behavior theories.
2. Draft logic model creation method
2.1 Creation procedure
In the cause-and-effect relationship chain among a program’s elements, each cause-and-effect relationship must have sufficient plausibility. This plausibility can only be provided by a theory showing that such a chain can occur in reality4). Therefore, we performed an extensive investigation on health behavior theories and models. We identified three theories and one model that would provide the basis for considering the outcomes and the logic to create a logically plausible draft model. The next section provides some details of the identified theories and model.
2.2 Health behavior-related theories and model investigated
The term “health behavior” refers to both health-promoting and health-demoting behaviors16). This study covered programs aiming at health promotion or lifestyle-related disease prevention. Hence, the present paper uses “health behavior” to refer to behaviors helpful for health promotion or lifestyle-related disease prevention. Besides, this paper principally discusses behaviors during behavior changes in the health field and, therefore, may use the word “behaviors” to mean “health behaviors.”
This study incorporated three theories and one model, each outlined below, from among various health behavior theories and models. The Social Cognitive Theory (SCT), the Transtheoretical Model (TTM), and the Health Belief Model (HBM) are most widely used in health behavior research and practice while the Ecological Model can supposedly complement the shortcomings of Social Cognitive Theory (SCT)16). The following subsections present the investigation findings on the theories and model.
2.2.1 Social Cognitive Theory (SCT)
The Social Cognitive Theory (SCT) aims at changing three factors (behavioral, cognitive, and environmental factors) to change health behaviors to prevent diseases or premature deaths. Behavioral factors include the ability to perform behaviors well, an intention to change behaviors, and rewards or punishments for behaviors. Cognitive factors include knowledge about behaviors, expectations, or anxieties for the consequences of behaviors, and self-efficacy in performing behaviors. Environmental factors refer to lessons learned from other people’s behaviors, feelings about surrounding people’s reactions to one’s behaviors, support from other people, and influences from social and physical environments16).
The SCT theory is primarily interested in behavior changes at the individual level and tends not to pay sufficient attention to environmental factors’ influences16). Therefore, this theory is used in combination with the Ecological Model to consider environmental factors in behavior changes.
2.2.2 Ecological Model
According to the Ecological Model, health behaviors are affected by factors at multiple levels, including intrapersonal, interpersonal, organizational, community, and public policy levels. When an environment or a policy impedes healthy behaviors, no effects can be expected from enhancing individuals’ motivation or skills for behavior change16). For example, as shown in obesity diagrams18), complicated interactions exist between food and the body and other various factors, such as education or the media.
2.2.3 Transtheoretical Model (TTM)
The Transtheoretical Model (TTM), which has evolved from a psychoanalysis theory, intends to explain how individuals reach a behavior change. A behavior change unfolds through the six stages of precontemplation, contemplation, preparation, action, maintenance, and termination. This unfolding process, however, does not always smoothly proceed in a one-way direction but may involve reversions from any one stage back to a preceding stage16).
2.2.4 Health Belief Model (HBM)
The Health Belief Model (HBM) includes elements useful for predicting whether and why individuals perform behaviors necessary to avoid, detect, and control illnesses. The main elements are perceived susceptibility, perceived severity, perceived benefits, perceived barriers, cue to action, and self-efficacy. These six elements can be described as follows, respectively: a perceived possibility of becoming ill or unhealthy’ a perceived severity of a disease left untreated’ perceived benefits from behaviors’ anticipated barriers to behavior engagement or perceived likelihood of possible undesirable results’ possible triggers to behaviors’ and self-confidence in performing health behaviors successfully16).
2.3 Outcomes and logic considered
Based on the prerequisites and the investigation findings mentioned above, we considered the outcomes constituting the draft model and the logic connecting them. When considering the outcomes and the logic, we kept in mind mainly the following two points: the first point was to determine the outcomes retrospectively from the long-term outcome6) to prevent logical leaps in the outcomes and logic for achieving the long-term outcome; and the second point was to configure the outcomes and logic based on the theories, model, and prerequisites mentioned above16).
The outcomes consisted of outcome categories of high abstraction degree and more detailed items included therein, in other words, detailed outcomes. The outcome categories were determined based mainly on the prerequisites specified for draft model creation and the combination of the theories and model collected through the investigation. Besides the components of the theories and model, items assuming an actual program were incorporated into the detailed outcomes. In what follows, however, both the outcome categories and the detailed outcomes are collectively called the “outcomes,” if the former and the latter require no hierarchical distinction for explanation purposes.
3. Results of draft logic model creation
The draft model we created is based on the investigation findings in the scope presented in Subsection 1.3. This draft model is an organized arrangement of outcomes and logic with which a program aiming at health promotion or lifestyle-related disease prevention through the use of healthcare-related products or services contributes to an extended healthy life expectancy of program participants (individuals). Subsection 3.1 explains the outcome components, while the detailed outcomes belonging thereto are presented in Subsection 3.2.
3.1 Overview of the outcome components
First, based on the prerequisites and the investigation findings mentioned above) we identified perspectives to be incorporated into the draft model. Then, we roughly specified the outcome components from the following four perspectives based on the above health behavior theories and model and the definition of “healthcare” in this study. Fig. 2 shows the overview of the outcome components as arranged correspondingly to the model finally obtained.
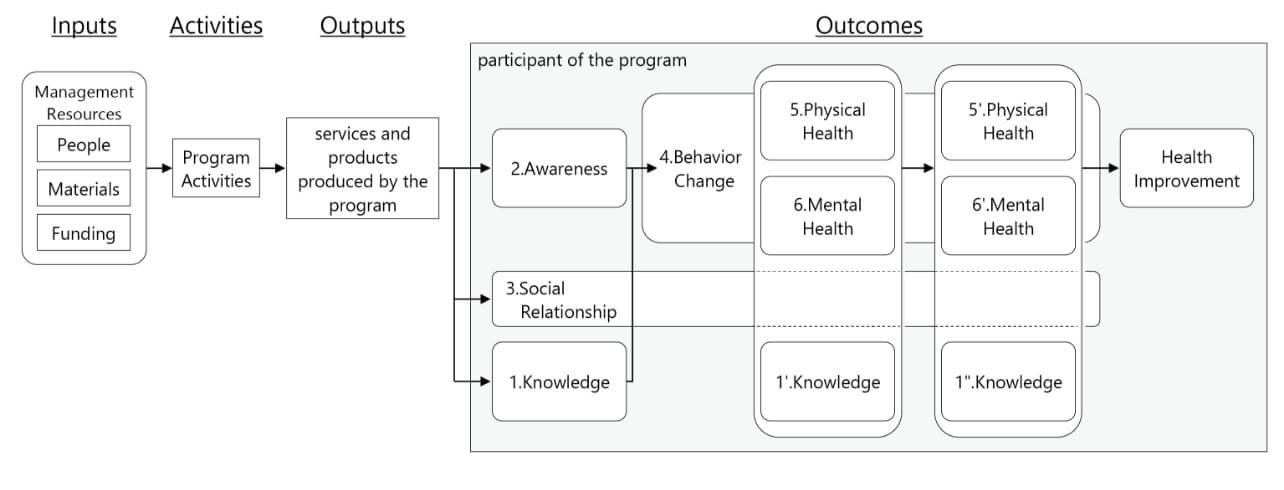
The first perspective incorporated into our model relates to health. In line with the content of healthcare in the sense defined for this study, the three of Outcome 5 “Physical Health,” Outcome 6 “Mental Health,” and Outcome 3 “Social Relationship” are set as the outcome components.
The second perspective is the axis for health-related behavior changes. This perspective is based on the Transtheoretical Model (TTM) and the Health Belief Model (HBM). An extended healthy life expectancy requires continued healthy behaviors, and a behavior change proceeds in stages. Therefore, Outcome 4 “Behavior Change” for health behaviors is placed at our model’s core. Our model is configured to allow individuals to achieve health improvement by going through the stages of behavior change while deepening their health beliefs.
The third perspective is the level that affects behaviors. This perspective is based on the Ecological Model. Outcome 3 “Social Relationship” is set as an outcome that affects behaviors at the environmental level. Meanwhile, Outcome 5 “Physical Health,” Outcome 6 “Mental Health,” and Outcome 1 “Knowledge” are set as outcomes that affect behaviors at the individual level.
The fourth perspective relates to behavior-affecting factors. This perspective is based on the Social Cognitive Theory (SCT) and the Health Belief Model (HBM) and reflects the fact that behavior-affecting factors include behavioral, cognitive, and environmental factors and behavior beliefs. Therefore, Outcome 1 “Knowledge,” Outcome 2 “Awareness,” Outcome 3 “Social Relationship,” Outcome 5 “Physical Health,” and Outcome 6 “Mental Health” are set as elements affecting Outcome 4 “Behavior Change.” We kept this perspective in mind when considering the detailed outcomes.
3.2 Determining individual outcomes and the logic connecting them
Based on the outcome components presented in Section 3.1, the detailed outcomes were determined together with the logic. Fig. 3 shows the obtained results. Note, however, that Fig. 3 shows only the outcomes excerpted from the logic model’s components. What follows explains Outcome Categories 1 to 10 along with the detailed outcomes belonging thereto. It should be noted, however, that some outcome names may appear abbreviated or modified depending on the explanatory content.
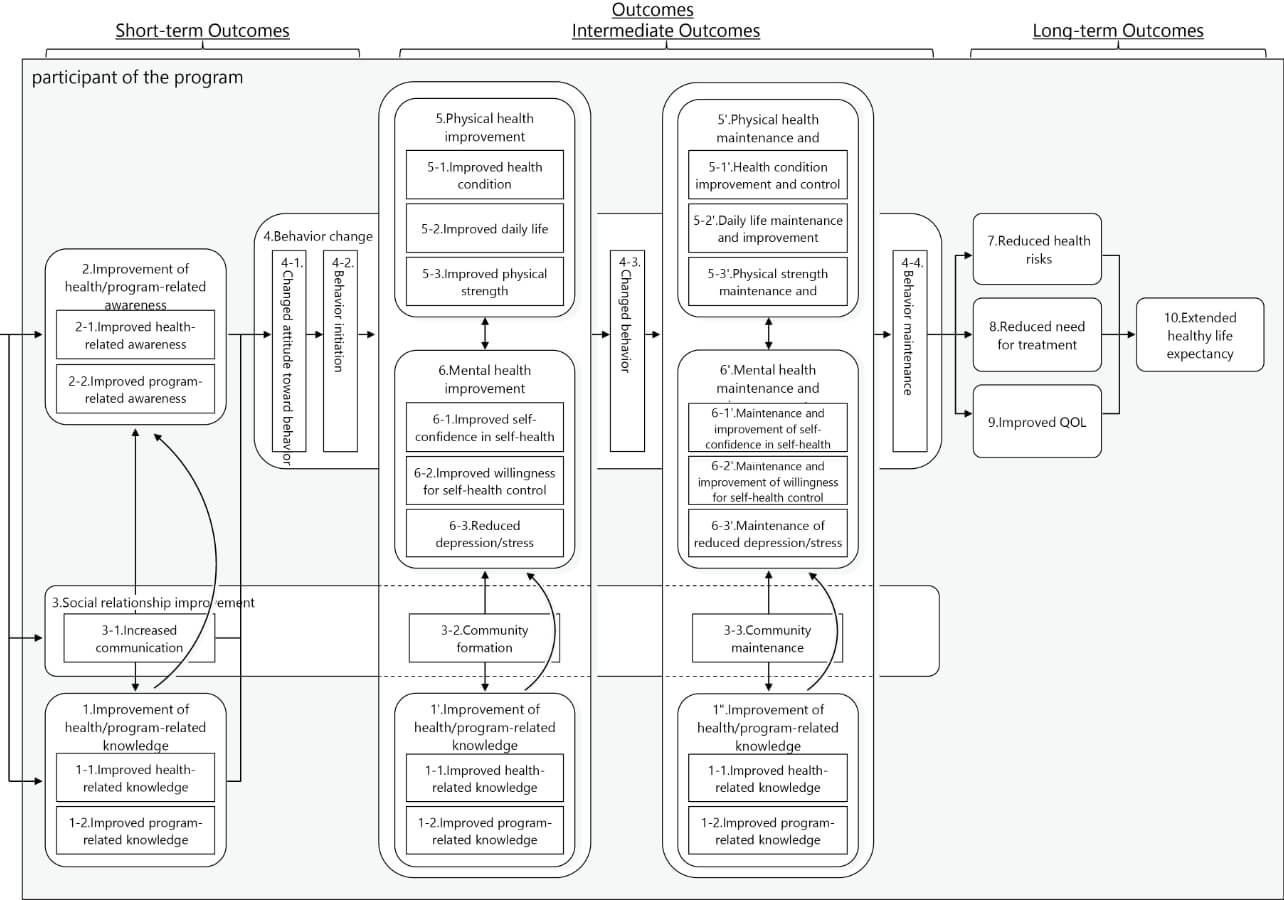
(1) Improvement of health/program-related knowledge
One of the outcomes directly resulting from program provision is Outcome 1 “Improvement of health/program-related knowledge.” The detailed outcomes belonging to this category are Detailed Outcome 1-1 “Improved health-related knowledge” and Detailed Outcome 1-2 “Improved program-related knowledge.”
These outcomes occur as a result of information provision from the program or individuals’ voluntary information collection and manifest themselves according to the stages of Outcome 4 “Behavior change” to promote a behavior change. For each behavior change stage in our model, the outcomes are numbered, for example, as 1, 1ʹ, and 1ʺ.
The provision of program-related information leads to Detailed Outcome 1-2 “Improved program-related knowledge.” Then, the program is better understood, thereby leading to Outcome 4 “Behavior change.” Meanwhile, the provision of health-related information leads to Detailed Outcome 1-1 “Improved health-related knowledge.” Improvement in health-related and program-related knowledge leads to positive effects on daily life behaviors. Examples of such information include information on the program’s effects, the risks of remaining in an unhealthy condition, and the degree of acceptability of individuals’ behaviors to their community. Outcome 1 “Knowledge improvement” also leads to Outcome 2 “Awareness improvement.” Information acquisition from a community through Outcome 3 “Social relationship improvement” also leads to Outcome 1 “Knowledge improvement.”
(2) Improvement of health/program-related awareness
Another outcome directly resulting from program provision is Outcome 2 “Improvement of health/program-related awareness.” The detailed outcomes are Detailed Outcome 2-1 “Improved health-related awareness” and Detailed Outcome 2-2 “Improved program-related awareness.”
Program provision leads to paying attention to the program and associated health issues. Not only does this Outcome 2 “Awareness improvement” directly result from program participation, but it may be influenced by Outcome 1 “Knowledge improvement” or Outcome 3 “Social relationship improvement.”
(3) Social relationship improvement
The outcome resulting from program provision and affecting behaviors at the environmental level is Outcome 3 “Social relationship improvement.” The detailed outcomes are Detailed Outcome 3-1 “Increased communication,” Detailed Outcome 3-2 “Community formation,” and Detailed Outcome 3-3 “Community maintenance.”
These outcomes are expected to manifest themselves after program provision and evolve, along with a behavioral change over time. Increased interpersonal involvements and social interactions will lead to exposure to information possessed by others or their sense of values, thereby resulting in improvement in individuals’ knowledge (Outcome 1) and awareness (Outcome 2). Besides, community membership provides individuals with access to support for performing health behaviors and may also motivate them to continue their health behaviors.
Thus, Outcome 3 “Social relationship improvement” not only has direct effects on Outcome 4 “Behavior change” through environmental improvement but also indirectly induces a behavior change through its effects on individuals’ knowledge (Outcome 1) or awareness (Outcome 2) and willingness (Detailed Outcome 6-2).
(4) Behavior change
Outcome 4 “Behavior change” manifests itself through Outcome 1 “Knowledge improvement,” Outcome 2 “Awareness improvement,” or Outcome 3 “Social relationship improvement.” The detailed outcomes are Detailed Outcome 4-1 “Changed attitude toward behavior,” Detailed Outcome 4-2 “Behavior initiation,” Detailed Outcome 4-3 “Changed behavior,” and Detailed Outcome 4-4 “Behavior maintenance.”
First, the initiation of any behavior requires a changed attitude toward it as its preceding stage. An individual initiates a behavior when their attitude becomes positive toward a behavior, in other words, when they expect that performing the behavior will lead to an outcome valuable to them. Then, their habitual behavior changes along with a health-related personal or environmental change. As a result, their health also begins to change and then proceeds to the behavior maintenance stage. However, it should be noted that a behavior change does not always proceed smoothly but may involve reversions from one stage back to a preceding stage.
(5) Physical health improvement/Physical health maintenance and improvement
This outcome undergoes a transition from improvement to maintenance and improvement between before and after Detailed Outcome 4-3 “Changed behavior.” Detailed Outcome 4-3 “Changed behavior” means a change in habitual behavior. A tentative behavior initiation alone is unlikely to lead to physical health maintenance. Hence, Outcome 5 “Physical health improvement” occurs before a change in behavior, after which a transition occurs to Outcome 5’ “Physical health maintenance and improvement.”
The detailed outcomes also change in content before and after the behavior change. Before the behavior change, they are Detailed Outcome 5-1 “Improved health condition,” Detailed Outcome 5-2 “Improved daily life,” and Detailed Outcome 5-3 “Improved physical strength.” After behavior change, they are Detailed Outcome 5-1’ “Health condition improvement and control,” Detailed Outcome 5-2’ “Daily life maintenance and improvement,” Detailed Outcome 5-3’ “Physical strength maintenance and improvement.” Detailed Outcome 5-1 “Health condition” in the sense used here includes subjective sensations, such as physical pain or physical conditions. Detailed Outcome 5-2 “Daily life” relates to daily life’s actions and tasks. Detailed Outcome 5-3 “Physical strength” is an item that directly affects the active waking hours and the walkable distance.
Outcome 5 consists of the three perspectives of changes in physical health condition (Detailed Outcome 5-1) through behaviors, daily life (Detailed Outcome 5-2) variable depending on the resulting condition, and physical strength (Detailed Outcome 5-3). Outcome 5 “Physical health” interacts with Outcome 6 “Mental health” explained below. The following two scenarios are possible: Outcome 6 “Mental health improvement” achieved through Outcome 5 “Physical health improvement” or the other way around. Their interactions promote Outcome 4 “Behavior change.”
(6) Mental health improvement/Mental health maintenance and improvement
Similarly to Outcome 5 “Physical health,” this outcome undergoes a transition from “Improvement” to “Maintenance and Improvement” between before and after Detailed Outcome 4-3 “Changed behavior.” The idea is to change habitual behavior to maintain and further improve mental health.
The detailed outcomes before the behavior change are Detailed Outcome 6-1 “Improved self-confidence in self-health control,” Detailed Outcome 6-2 “Improved willingness for self-health control,” and Detailed Outcome 6-3 “Reduced depression/stress.” The detailed outcomes after the behavior change are Detailed Outcome 6-1’ “Maintenance and improvement of self-confidence in self-health control,” Detailed Outcome 6-2’ “Maintenance and improvement of willingness for self-health control,” Detailed Outcome 6-3’ “Maintenance of reduced depression/stress.”
The self-health control-related self-confidence and willingness (Detailed Outcomes 6-1 and 6-2) relate to the intention to perform behaviors. Self-confidence in performing health-promoting behaviors independently, coupled with a willingness to become healthy by doing so, leads to performing such behaviors in reality. A depressed/stressed state (Detailed Outcome 6-3) is a manifestation of an individual’s mental health condition.
Mental health (Outcome 6) is affected by a community with a shared objective, in other words, by social relationship (Outcome 3) or knowledge (Outcome 1), and interacts with physical health (Outcome 5).
(7) Reduced health risks
Outcome 7 “Reduced health risks” is one of the outcomes that result from healthy behavior maintenance (Detailed Outcome 4-4) and lead to an extended healthy life expectancy (Outcome 10). Improved physical and mental health (Outcomes 5 and 6), improved social relationship (Outcome 3), and improved knowledge (Outcome 1), coupled with the behavior maintenance therefor (Detailed Outcome 4-4), reduce the possibility of occurrence of diseases and other health-related problems.
Physical health condition (Detailed Outcome 5-1) and depressed/stressed state (Detailed Outcome 6-3) are the determining factors for health risks (Outcome 7). Then, Outcome 7 Reduced health risks is achieved by behavior maintenance (Detailed Outcome 4-4) through improved daily life (Detailed Outcome 5-2), improved physical strength (Detailed Outcome 5-3), improved self-confidence or willingness (Detailed Outcomes 6-1 and 6-2), improved social relationship (Outcome 3), and improved knowledge (Outcome 1).
(8) Reduced need for treatment
Outcome 8 “Reduced need for treatment” is the second outcome that results from Detailed Outcome 4-4 “Behavior maintenance” and leads to Outcome 10 “Extended healthy life expectancy.” Improved physical health and mental health (Outcomes 5 and 6) reduce the required frequency or number of times of treatment. Consequently, medical costs also decrease. It is also probable that continued health behaviors will make treatment unnecessary.
(9) Improved QOL
Outcome 9 “Improved QOL” is the third outcome that results from Detailed Outcome 4-4 “Behavior maintenance” and leads to Outcome 10 “Extended healthy life expectancy.” QOL is the acronym for “quality of life.” A high QOL state means a state of living a lively life without any health condition problem.
Besides having no health condition problems (Detailed Outcome 5-1) and being in a non-depressed/stressed state (Detailed Outcome 6-3), behavior maintenance (Detailed Outcome 4-4) for good maintenance of the following leads to Outcome 9 Improved QOL: daily life (Detailed Outcome 5-2), physical strength (Detailed Outcome 5-3), self-confidence (Detailed Outcome 6-1), willingness (Detailed Outcome 6-2), and social relationship (Outcome 3).
(10) Extended healthy life expectancy
The long-term outcome of our model is Outcome 10 “Extended healthy life expectancy.” The achievement of physical, mental, and social health (Outcomes 5, 6, and 3) through a program, coupled with the behavior maintenance therefor (Detailed Outcome 4-4), lead to reduced health risks (Outcome 7), a reduced need for treatment (Outcome 8), and an improved QOL (Outcome 9). The subsequent outcome is an extended healthy life expectancy (Outcome 10). Outcome 10 “Extended healthy life expectancy” is not achievable in a short period but is expected to be achieved through behavior maintenance (Detailed Outcome 4-4).
3.3 Reliability of the draft model based on preceding studies
The draft model thus created was examined for reliability by comparison with preceding studies on healthcare programs. The aim was to confirm that the outcomes and logic derived from health behavior theories can occur in actual events but not to verify their frequency of occurrence and relative frequency. More specifically, we confirmed that a series of findings on program provision to utilization in two cases, one being a low-frequency therapy device and the other being an online diet program, did not conflict with our model’s outcomes and logic. The following subsections present these two cases’ details, with each detail appended with a corresponding outcome number in parentheses.
3.3.1 Case Study : Low-frequency therapy device
We (Omron Expert Link Co., Ltd.) compared our draft model with the case study19) we had conducted in 2016 on a home-use low-frequency therapy device. A low-frequency therapy device is an electric therapy device able to reduce stiffness or pain in the shoulder or waist by electrotherapy. In the study, a low-frequency therapy device was provided free of charge to each of ten general users (four males and six females in their 30s to 60s) with a high willingness to purchase a low-frequency therapy device in return for cooperation in long-term monitoring performed using the diary method and retrospective interviews. For this paper, we examined the subjects for any awareness change, behavior change, therapeutic effect, or any other occurrences by contrast with our draft model. The occurrence of the following outcomes was observed:
The subjects obtained knowledge about the therapy device from product information materials, the operating manual, and other sources (1-2). Considering their stiffness or pain conditions, the subjects became positive in their attitudes toward treatment (4-1) and began to use the therapy device (4-2). Although they initially began using the therapy device for cooperation in the study (2-2), the subjects experienced a real therapeutic effect (5-1 and 6-1), became more willing for treatment using the therapy device (6-2), and became its continuous users (4-3). It was observed that the continuous use of the therapy device produced the effect of a gradual decrease in stiffness/pain level (5-1’). As a result of this effect, in some cases, the subjects showed a virtuous circle of, for example, becoming more active in their daily life (5-2’), going out more frequently, and improving in health condition (5-1’ and 5-3’).
In some cases, thanks to the decrease in stiffness/pain level, the subjects were seen to become more active in their daily lives, enjoy more quality time with their family members, and improve their relationship with their family members (3-3). These results led the subjects to become self-confident in expanding the range of their activities through the use of the therapy device (6-1’), willing to become healthier (6-2’), and determined to keep using the therapy device (4-4). In some other cases, the subjects showed a decrease in the frequency of hospital visits for treatment (8).
3.3.2 Case Study: Online diet program
A preceding case study20) on an online diet program presented results applicable to our model. The case study reported the results of a 90-day online diet program offered to three program users (one female in her 20s, one male in his 40s, and another male in his 50s). Its findings were based on wearable device measurement logs (body weight, body fat ratio, activity amount, and sleep time and depth), diet check sheet records, ketone-body-level check sheet records, and online chatting logs. This program was conducted through three chat sessions a day with a physical therapist and an occupational therapist while the diet, exercise, and sleep status records of each user were individually shared. All three users showed decreases in body weight and body fat ratio. Each program user’s chat history was analyzed to identify contexts and utterances instrumental to behavior change. The contexts and utterances thus identified corresponded to the outcomes of this study’s draft model as follows:
It was observed that the program users paid attention to their eating habits (2-1 and 2-2) when they learned about the sugar contained in their diet (1-1 and 1-2). Consequently, they were seen to find and address challenges in their dieting (4-1 and 4-2). Some situations were observed in which after experiencing a decrease in body weight (5-1) through short-term dietary improvement (4-2), the program users began to reconsider the balance between their activity amounts and diet (4-3). It was also observed that the 90-day program led them to understand the relationship of body weight increase and decrease to exercise and diet (5-1’, 5-2’, and 1”) and become self-confident in continuously controlling body weight (6-1’). There were also situations in which they were observed to learn about proper eating methods through chat exchanges with the physical therapist and the occupational therapist (1, 1’, and 1”) and to try putting the taught methods into practice (6-2 and 6-2’).
4. Conclusions
In this study, we created a draft logic model based on three health behavior theories and one health behavior model to ensure that the programs aiming at health promotion or lifestyle-related disease prevention through the use of healthcare-related products or services contribute to an extended healthy life expectancy of program participants (individuals). This draft logic model will provide a template for creating logic models for healthcare-related programs, thus reducing planning workloads. Besides, we expect our model to help solve healthcare program-related social issues as used and improved in actual programs. We concluded that our study thus contributes to resolving social issues as support for social issue-solving efforts by enterprises and organizations, including OMRON.
It should be noted that a simplified version of our study’s model has been made publicly available as a social impact measurement toolset for healthcare together with typical outcome measurement indicators20). Released by SIMI, this simplified version is intended for widespread use by NPOs and social enterprises.
The model we created has been verified only for usefulness by comparison with preceding studies and hence requires further verification and improvement through actual use. We intend to improve our model through verification for applicability to other cases and actual programs.
We will consider expanding the scope of the draft logic model to improve it. In 1998, a proposal was made for adding the word “spiritual” to the WHO’s definition of health but failed to reach adoption. The proposal was made from the perspective that the word “spiritual” can be paraphrased as “mental” or “incorporeal”21) and hence is necessary and essential to consider the securement of human dignity and the quality of life22). Spiritual areas fall outside the scope of this study. Nevertheless, as suggested by the SINIC Theory23), a social sense of values will grow that attaches importance to psychological satisfaction and individuals’ ways of life, and needs will emerge of the development of human-related sciences and technologies interested in human qualities, such as intellect and sensibilities. In the foreseeable future, logic models will become necessary which serve the needs of such a mature society and contribute to solving healthcare program-related social issues. Therefore, one of our future challenges lies in creating a draft model for health, including its spiritual aspects. In this paper, we have avoided discussing incentives in the form of monetary or point rewards. However, these incentives are among the possible factors influential on health behavior changes. Hence, we will take these points into account to expand our model.
References
- 1)
- Social Impact Measurement Working Group of the GSG National Advisory Board, Practical Manual for the Social Impact Measurement Toolset, Ver. 2.0 (in Japanese), Social Impact Management Initiative, 2017, 39 p., http://www.impactmeasurement.jp/pdf/NAB_manual_ver2.pdf (accessed Dec. 20, 2019).
- 2)
- Deliberation Working Group on Social Impact Measurement, Toward the Promotion of Social Impact Measurement ‒ Social Impact Measurement for Solving Social Issues: Basic Concepts and Future Measures (in Japanese), Cabinet Office, 2016, 42 p., https://www.npo-homepage.go.jp/uploads/social-impact-hyouka-houkoku.pdf (accessed Dec. 20, 2019).
- 3)
- Social Impact Management Initiative Joint Secretariat, “SIMI Social Impact Management Initiative” (in Japanese), SIMI/Social Impact Management Initiative, http://www.impactmeasurement.jp/ (accessed Dec. 20, 2019).
- 4)
- P. H. Rossi, M. W. Lipsey, and H. E. Freeman, Evaluation: A Systematic Approach (Japanese translated version), Tokyo: Nippon Hyoron Sha Co., Ltd., 2005, 418 p.
- 5)
- Y. Minamoto, Qualitative Improvement and Evaluation of Policies ~ Through Application of Program Evaluation Theory ~, Outline of Unified Workshop (Central Workshop) on Policy Evaluation (in Japanese), Ministry of Public Management, Home Affairs, Posts, and Telecommunications, 2017, 36 p., https://www.soumu.go.jp/main_content/000474081.pdf (accessed Dec. 20, 2019).
- 6)
- Nippon Foundation, Logic Model Creation Guide (in Japanese), Nippon Foundation Operational Secretariat for Social Innovation Award 2019, 10 p., https://www.nippon-foundation.or.jp/app/uploads/2018/12/wha_pro_sif_rec_02.docx (accessed Dec. 20, 2019).
- 7)
- Agriculture, Forestry, and Fisheries Policy Information Center of Agriculture, Forestry and Fisheries Promotion Foundation, Logic Model Development Guide (in Japanese), Agriculture, Forestry, and Fisheries Research Institute, 2003, 82 p., https://www.maff.go.jp/primaff/about/center/hokoku/attach/pdf/200308_hk066.pdf (accessed Dec. 24, 2019).
- 8)
- PricewaterhouseCoopers Arata LLC, Highly Evaluated Cases (in Japanese), Cabinet Office, 2017, 43 p., https://www.npo-homepage.go.jp/uploads/h28-social-impact-sokushin-chousa-04.pdf (accessed Dec. 25, 2019).
- 9)
- K-Three Inc., Demonstration Project Results Report: Kanagawa Prefecture SDGs Social Impact Evaluation and Demonstration Project (Evaluation Worksheets Collection) (in Japanese), Kanagawa Prefecture, 2019, 71 p., http://www.pref.kanagawa.jp/docs/bs5/documents/3.pdf (accessed Dec. 25, 2019).
- 10)
- Saga Prefecture, The Seventh Saga Prefecture Health Care Plan (in Japanese), Saga Prefecture, 2018, https://www.pref.saga.lg.jp/kiji00361067/3_61067_94107_up_esm7csie.pdf (accessed Jan. 9, 2020).
- 11)
- Okinawa Prefecture, The Seventh Okinawa Prefecture Healthcare Plan (in Japanese), Okinawa Prefecture, 2018, https://www.pref.okinawa.jp/site/hoken/iryoseisaku/kikaku/documents/dai5.pdf (accessed Jan. 9, 2020).
- 12)
- Investigative Committee for Promotion of Research and Development Evaluation, Office for Evaluation and Research and Development Corporation Support, Planning and Evaluation Division, Science and Technology Policy Bureau, Ministry of Education, Culture, Sports, Science and Technology, Logic Model Creation Workshop (in Japanese), Ministry of Education, Culture, Sports, Science and Technology, 2018, 14 p., https://www.mext.go.jp/component/a_menu/science/detail/__icsFiles/afieldfile/2018/12/11/1411585_02.pdf (accessed Dec. 25, 2019).
- 13)
- Secretariat of the Next-Generation Healthcare Industry Council (Ministry of Economy, Trade, and Industry), On the Future Directions for the Next-Generation Healthcare Industry Council (in Japanese), Ministry of Economy, Trade, and Industry, 2018, 27 p., http://warp.da.ndl.go.jp/info:ndljp/pid/11169867/www.meti.go.jp/committee/kenkyukai/shoujo/jisedai_healthcare/pdf/007_02_00.pdf (accessed Dec. 25, 2019).
- 14)
- Ministry of Health, Welfare, and Labour, Vision for 2040 Aiming at Realizing a Society Where Everyone Can Live a Long Active Healthy Life (Healthcare Delivery System Reform With a View to 2040, Promotion of Data Health Reform, and Support for Further Expanding Job Opportunities for the Employment Ice Age Generation) (in Japanese), Cabinet Office, 2019, 10 p., https://www5.cao.go.jp/keizai-shimon/kaigi/minutes/2019r/0531/shiryo_02.pdf(accessed Dec. 25, 2019).
- 15)
- Public interest incorporated association Friends of WHO JAPAN, “On the Definition of Health” (in Japanese), Public interest incorporated association Friends of WHO JAPAN, https://www.japan-who.or.jp/commodity/kenko.html (accessed Dec. 25, 2019).
- 16)
- K. Glanz, and B. K. Rimer, Health Behavior: Theory, Research, and Practice (Japanese translated version), Medical Science International, 2018, 427 p.
- 17)
- C. Matsumoto, Foundations of Health Behavior Theory for Medical and Healthcare Staff: Focusing on Lifestyle-Related Diseases (in Japanese), Ishiyaku Publishing, Inc., 2002, 100 p.
- 18)
- Government Office for Science, Tackling Obesities: Future Choices – Project Report, 2nd ed., GOV. UK, 2007, 161 p., https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/287937/07-1184x-tackling-obesities-future-choices-report.pdf(accessed Dec. 25, 2019).
- 19)
- Social Impact Management Initiative Outcome Indicator Working Group, Social Impact Measurement Toolset for Healthcare, Ver. 1.0 (in Japanese), SIMI Social Impact Management Initiative, 2019, 40 p., http://www.impactmeasurement.jp/wp/wp-content/uploads/NAB_healthcare_ver1.pdf(accessed Dec.27, 2019).
- 20)
- K. Yoshida, Y. Morimoto, A. Aoki, and K. Eguchi, “Variety of Behavioral Change through Internet-Based Intervention for Obesity.” (in Japanese), General Rehabilitation, vol.1, pp. 39-45, 2019.
- 21)
- Sanseido, “Spiritual,” Sanseido Web Dictionary (in Japanese), https://www.sanseido.biz/User/Dic/Index.aspx?TWords=spiritual&st=0&DORDER=&DailyJJ=checkbox&DailyEJ=checkbox&DailyJE=checkbox(accessed Jan. 10, 2020).
- 22)
- International Affairs Division, Minister’s Secretariat Ministry of Health, Labour and Welfare, “On the Revision Proposal for the Definition of ‘Health’ in the WHO Constitution” (in Japanese), Ministry of Health, Welfare, and Labour, https://www.mhlw.go.jp/www1/houdou/1103/h0319-1_6.html (accessed Dec. 25, 2019).
- 23)
- OMRON Corporation, Integrated Report 2016 (in Japanese), OMRON Japan, 2016, pp. 56-57, https://www.omron.co.jp/ir/irlib/pdfs/ar16j/ar2016j.pdf(accessed Dec. 25, 2019).
The names of products in the text may be trademarks of each company.
















